What Is Breast Implant Illness? – a Social Media Phenomenon or a Real Condition?
Breast implant surgery is one of the most popular cosmetic procedures in the world.
Increased breast size and improved silhouette are just some of the many advantages of the boob job or breast augmentation.
However, lately, we have witnessed the rise of concerns regarding this procedure. Many women express their worries about breast implant illness on social media. You can read all sorts of claims online, but it’s difficult to determine what’s real or not. In this post, we are going to walk you through breast implant illness and provide the answers you’re looking for.
What is breast implant illness?
Breast implant illness (BII) is a term that refers to various symptoms that may develop after undergoing cosmetic augmentation or reconstruction with breast implants. Although BII has become a widely talked about subject today, the link between breast implants and systemic disease has been reported since the 1960s, according to a study from the Plastic and Reconstructive Surgery Journal. Also referred to as autoimmune/inflammatory syndrome induced by adjuvants (ASIA), it is a constellation of symptoms, unbound by a single organ system, which begins after the placement of implants.
Although BII was reported decades ago, it’s still a controversial subject. Social media is swamped with posts and claims about BII, and many of them are laden with false information. Additionally, BII is a subject of debates among plastic surgeons as they disagree on whether the condition is real or symptoms are a result of something else. Cosmetic surgeons across the globe are working on different studies regarding BII to determine how symptoms develop, find the best treatment approach, and learn as much as possible about all the underlying mechanisms.
Breast implant illness can develop regardless of whether you have saline, gel, smooth, or textured implants.
It’s important to mention that, at this point, BII is not a medically recognised condition due to a lack of studies that focus on it as a unique condition. Improvements in this aspect are evident, though. In March 2019, the U.S. Food and Drug Administration (FDA) organised a panel to discuss the risks and benefits of breast implants used for breast augmentation and reconstruction. The panel also addressed BII. In September 2020, the FDA issued a statement wherein they recommend a format and content changes to breast implant labelling, so the information is presented in an understandable manner. The importance of these black box warnings is so that patients can discuss both benefits and risks of breast implants.
Why does breast implant illness happen?
The exact mechanism of BII is still unknown. However, multiple theories suggest the symptoms occur due to an inflammatory process triggered by the introduction of silicone. A lot more research on this subject is necessary to uncover why BII happens. Other hypotheses include human adjuvant disease, silicone-induced incompatibility syndrome, ASIA, heavy metal poisoning associated with implant manufacture (or even tattoos), and chronic inflammation/infection or allergy caused by yeasts in saline implants and around implants.
Moreover, some women could be predisposed to having an immune reaction to the materials that are used to manufacture breast implants. This creates inflammation that induces the symptoms of BII.
What are the symptoms of breast implant illness?
Breast implant illness is associated with a wide spectrum of symptoms. The exact symptoms may vary from one woman to another. However, in most cases, women with BII experience:
- Fatigue
- Brain fog
- Joint pain
- Anxiety
- Hair loss
- Depression
- Rash
- Autoimmune disease
- Inflammation
- Weight fluctuation
Other symptoms of BII may include numbness and tingling in extremities, dry eyes and/or blurred vision, breast pain, muscle pain, food sensitivity/intolerance, flu-like symptoms, and/or low-grade fever, low libido, and difficulty breathing. In fact, over 100 symptoms could be associated with BII, but keep in mind they can also occur due to other causes such as fibromyalgia, non-autoimmune hypothyroidism, IBS, among others. Having the above-mentioned symptoms does not automatically indicate you have BII, but you may want to consult your surgeon.
How do you test for breast implant illness?
Since BII is not recognised as a formal medical diagnosis, there is no specific test or criteria to define or characterise this constellation of various symptoms. Women with BII often have a wide range of symptoms and may see their doctor regarding the symptoms before realising they could be connected with their implants. The story is different for everyone. At this point, the only way for a surgeon to determine you have BII is to rule out other potential causes of the symptoms you experience.
How is breast implant illness treated?
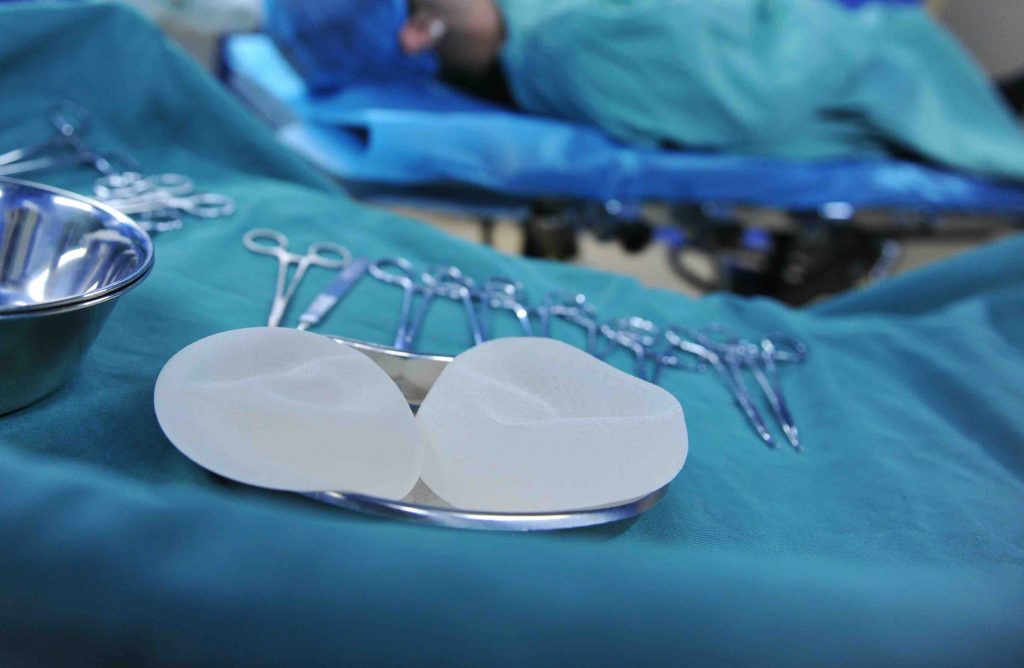
Every surgeon may have a different approach toward addressing BII in their patients.
The journal Annals of Plastic Surgery published a retrospective study of all patients who underwent explantation by a single surgeon over two years. A total of 750 patients met the inclusion criteria. The study showed that patients presenting with symptomatic BII had significant immediate improvement in 11 common symptoms after the removal of the implant and capsule. But scientists emphasise the need for further research on this subject, especially studies inspecting long-term results.
Just like BII itself, the treatment is also a subject of many debates. “En bloc” capsulectomy (removal of both the implant and the capsule in one piece) is often mentioned as the ideal approach. Dr Mark Doyle has over 30 years of experience as a qualified plastic surgeon and regularly uses the En Bloc technique when performing breast implant removal surgery.
“I believe in this approach and have removed several hundred implants for patients with BII. The majority of patients treated have dramatic improvements in their symptoms.
“Currently, we just don’t know enough about the condition. My personal approach is simple. When a foreign body like a breast implant is placed inside the body, the bodies reaction is to form scar tissue around the implant to “protect” the body. It would appear logical that the potential cause of the BII may be related to one or more of the following – the implant, something on the surface of the implant or the capsule. If all of these items are removed in one piece this means there is no exposure of the body to any contaminants on the surface of the implant. And, if the implants in question have a textured surface then the complete removal of the capsule will remove the risk of the growth of a Lymphoma (ALCL) in the capsule,” says Dr Mark.
En bloc removal is a more invasive procedure that requires longer operative time and larger incision. The procedure also carries surgical risks such as hematoma, pneumothorax (collapsed lung), and potential deformity in women with thin tissues. These risks are well known and can be avoided by meticulous surgery.
This is not an operation that should be undertaken by inexperienced surgeons.
Before explantation, it is important to rule out other causes that may induce the same symptoms as BII. This may include complete blood count, thyroid function, liver, and renal function, and breast imaging as indicated. Once other potential causes are ruled out then implant removal will be recommended.
Many patients get information about BII from social media, not surgeons. As a result, they don’t get reliable and accurate information which can prevent them from getting adequate treatment for their condition regardless of the underlying cause.
FAQs
How common is breast implant illness?
At this point, there are no official statistics regarding the actual number of BII cases. Online communities count thousands of members who share their experiences with breast implant illness. Further research is necessary not only to elucidate mechanisms of action but also to uncover the prevalence and incidence of BII in Australia and worldwide.
What happens if you don’t replace breast implants?
Breast implants are medical devices, and you may need to have them remove or replaced at some point in the future. Some women can have the same implants for up to 10 years or even longer, but others don’t. It’s important to see your surgeon for checkups. Failing to replace a breast implant when it’s necessary can cause serious complications such as implant rupture.
Does insurance cover breast implant illness?
Since breast implant illness is not officially recognised as a medical condition, the chances of insurance covering it are small. Also, health insurance plans usually don’t cover the cosmetic procedures and may not want to provide coverage for side effects of that surgery. If you have issues with breast capsules often medicare item numbers do apply.
What do I do if my breast implants have been recalled?
The Therapeutic Goods Administration (TGA) has recalled a number of breast implants within Australia due to concerns relating to BIA-ALCL. The recall requires all plastic and cosmetic surgeons to return un-implanted stock, and these devices can no longer be supplied, imported or exported from Australia. If you have any of the recalled breast implants, the TGA recommends that you don’t need to do anything except be aware of the symptoms of BIA-ALCL and seek advice from a health professional if you notice any changes.
What are the long-term effects of breast implants?
Experiences of different women with breast implants vary. Some women may not have any long-term adverse reactions while others do. Capsular contracture and implant ruptures are the most common complications of breast implants.
Can breast implants cause autoimmune disorders?
Many symptoms of BII are also signs of various autoimmune conditions. A study from the Annals of Surgery analysed the long-term safety and efficacy of patients with breast implants. The study included 99,993 patients and found that silicone implants were linked with higher rates of Sjogren syndrome, scleroderma, rheumatoid arthritis, stillbirth, and melanoma. Sjogren syndrome, scleroderma, and rheumatoid arthritis are common autoimmune conditions. Keep in mind the study didn’t exactly say breast implants caused these autoimmune disorders. The research merely pointed to a higher prevalence of autoimmune disorders in women with breast implants. More studies are necessary to determine the nature of the connection between breast implants and autoimmune conditions.
Can breast implants cause weight gain?
It’s not uncommon to gain weight after a breast augmentation procedure. A small percentage of gained weight is due to implants, while the rest is down to factors associated with the procedure. Fluid retention is one of the most common factors that lead to weight gain after breast enlargement. The stress linked with a major surgery alongside medications prescribed for recovery may cause the body to retain fluid, thus contributing to weight gain. Other factors that play a role in gaining weight after boob job (breast augmentation) include swelling and lack of physical activity during recovery. This weight gain is transient and long term the only weight gain should be due to the extra weight of the implants.
Do breast implants cause heart problems?
The relationship between breast implants and heart function requires research. One study found that breast implants may impede ECG and lead to a false heart attack diagnosis. That happens because the implants may act as a barrier between the heart’s electrical activity and ECG electrodes. There is no evidence that breast implants and heart disease are associated.
Can breast implants cause hair loss?
Hair loss is a common symptom of BII. Generally speaking, anything that causes systemic reaction can contribute to hair loss, and that could happen with breast implant illness. More research is necessary to discover why, exactly, that happens.
Do breast implants cause brain fog?
Brain fog is one of the most common symptoms of BII. However, the relationship between breast implants and memory problems or poor concentration is unclear.
What happens to the capsule after implant removal?
The capsule is a scar tissue that forms due to a natural healing process upon implantation procedure. After all, a breast implant is a foreign body that incites a natural response. That’s why the body creates the barrier of scar tissue to envelope it and separate it from the rest of the body. A capsule is usually soft, filmy, and hardly noticeable, but in some women, it can become hard, painful, and tight like a shell. Explant alone leaves capsule in its place i.e. it is not removed.
What is the safest breast implant on the market?
Not all breast implants are equal; some are safer than others. The most reliable breast implants on the market are Motiva and Mentor. They are smooth, round, and secure, which is why the most reputable plastic surgeons tend to use these breast implants.
Bottom line
Breast implant illness has become a popular subject among social media users. Although the reports of symptoms occurring after breast implants have been reported since the 1960s there’s still a lot more we need to learn about it.
If you believe you are suffering from breast implant illness and wish to have your implants removed, book a consultation with Dr Mark Doyle, specialist plastic surgeon.
Related Blogs
- Will Medicare Cover My Breast Implant Removal in Queensland?
- What Is Breast Implant Malposition and Breast Implant Flipping?
- Rise in Breast Explants due to BIA-ALCL fears | GCPS
- Why Get an En Bloc Technique Breast Implant Removal
- What Is Breast Implant Illness? – a Social Media Phenomenon or a Real Condition?
- Nipple Reshaping and Areola Reduction: Who Is the Ideal Candidate, Benefits, and More
- Motiva Breast Implants and Why Dr Doyle Thinks They Are Best
References
- Breast Implant Illness: A Way Forward; Plastic and Reconstructive Surgery Journal
- Press Release – FDA Issues Final Guidance for Certain Labeling Recommendations for Breast Implants
- Understanding Breast Implant Illness, Before and After Explantation; Annals of Plastic Surgery
- Breast Implant Illness, Biofilm, and the Role of Capsulectomy; Plastic and Reconstructive Surgery Global Open
- US FDA Breast Implant Postapproval Studies; Annals of Surgery
- The Long-Term Outcomes of Breast Implants Studied; Medical News Today
- Breast implants may impede ECG and lead to false heart attack diagnosis; European Society of Cardiology
About Dr Mark Doyle FRACS (Plast) – Queensland Plastic Surgeon
Servicing patients in Gold Coast, Brisbane, Sunshine Coast, Cairns and New South Wales NSW – Northern Rivers, Byron Bay, Ballina, Lismore and more.
Dr Mark Doyle is a Specialist Plastic Surgeon with over thirty years of experience performing Breast, Body, Face and Nose surgery. Dr Doyle is a fully qualified Specialist Plastic Surgeon with 30+ years of experience. He has completed all required training and only carries out approved surgical practices. There are absolutely NO undertrained doctors or cosmetic doctors acting as surgeons in our clinic.
As a highly esteemed plastic surgeon, Dr Mark is committed to achieving the best possible results for all his breast, body, face and nose patients, both men and women.

